MIT Engineers Create Mini Liver to Test Disease Treatments
Scientists at MIT built a tiny working liver model that could revolutionize how we find treatments for liver disease affecting over 100 million Americans. The breakthrough offers hope for discovering drugs that actually work for everyone.
More than 100 million Americans live with fatty liver disease, but finding treatments that work has been frustratingly difficult. Now MIT engineers have created something that could change everything: a mini liver that works just like the real thing.
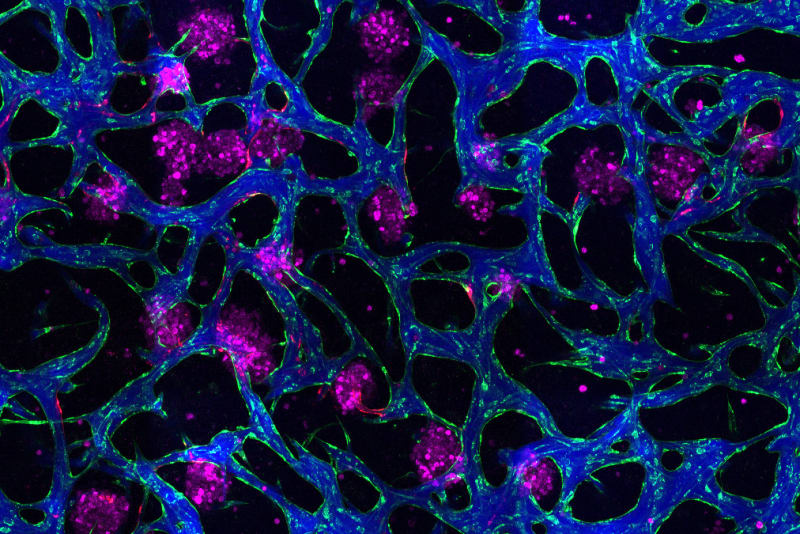
The new "liver-on-a-chip" is a tiny, functioning liver complete with blood vessels and immune cells. It's small enough to fit in your hand but sophisticated enough to show exactly how liver disease develops and how treatments might stop it.
The team found something surprising when they tested an existing liver drug called resmetirom. While the medication helps about 30 percent of patients, it can trigger inflammation in liver tissue, which may explain why it doesn't work for everyone. That's the kind of insight that's nearly impossible to get from traditional animal testing.
This matters because fatty liver disease can progress into more serious conditions with scarring and inflammation. Right now, only two medications are FDA-approved to treat advanced liver disease, and neither works for all patients.
The breakthrough builds on technology Professor Linda Griffith originally developed in the 1990s called the LiverChip. Pharmaceutical companies already use simpler versions to test whether new drugs might harm the liver, but this upgraded model does something more powerful: it recreates actual disease conditions.

To simulate fatty liver disease, the researchers exposed their mini liver to high levels of insulin, glucose, and fatty acids. The tissue responded just like a real liver would, developing fat buildup and insulin resistance.
The beauty of this approach is that researchers can now watch disease unfold in real time and test potential treatments at different stages. They can see which drugs might work best early in the disease versus later, and understand why some patients respond differently than others.
The Ripple Effect
This technology could speed up the search for new liver disease treatments dramatically. Instead of relying on animal models that don't always predict human responses, researchers can test drugs on tissue that behaves like an actual human liver.
The implications reach beyond liver disease too. The same approach could eventually help develop better treatments for other conditions where traditional testing falls short. Every drug that makes it through development faster means patients get help sooner.
For the millions of Americans living with liver disease and waiting for better options, this tiny chip represents something big: a faster path to treatments that actually work for their bodies.
Based on reporting by MIT News
This story was written by BrightWire based on verified news reports.
Spread the positivity!
Share this good news with someone who needs it