Stanford Finds Brain Circuit That Could End Chronic Pain
Scientists discovered a brain circuit that drives chronic pain independently from normal pain signals, opening the door to treatments that could help 60 million Americans without blocking protective pain responses. The breakthrough may finally separate relief from risk.
Scientists at Stanford University have mapped a hidden brain circuit that keeps chronic pain alive long after injuries heal, offering new hope for the nearly 60 million Americans trapped in cycles of persistent pain.
The discovery, published in Nature, reveals something researchers didn't expect. Acute pain and chronic pain travel completely separate pathways in the brain, meaning doctors could one day turn off long-term suffering without eliminating the body's alarm system for immediate danger.
"A surprise to us was that acute pain and chronic pain can be completely separate," said Xiaoke Chen, associate professor of biology at Stanford. His team found that silencing the chronic pain circuit stopped oversensitivity to touch while leaving normal pain detection fully intact.
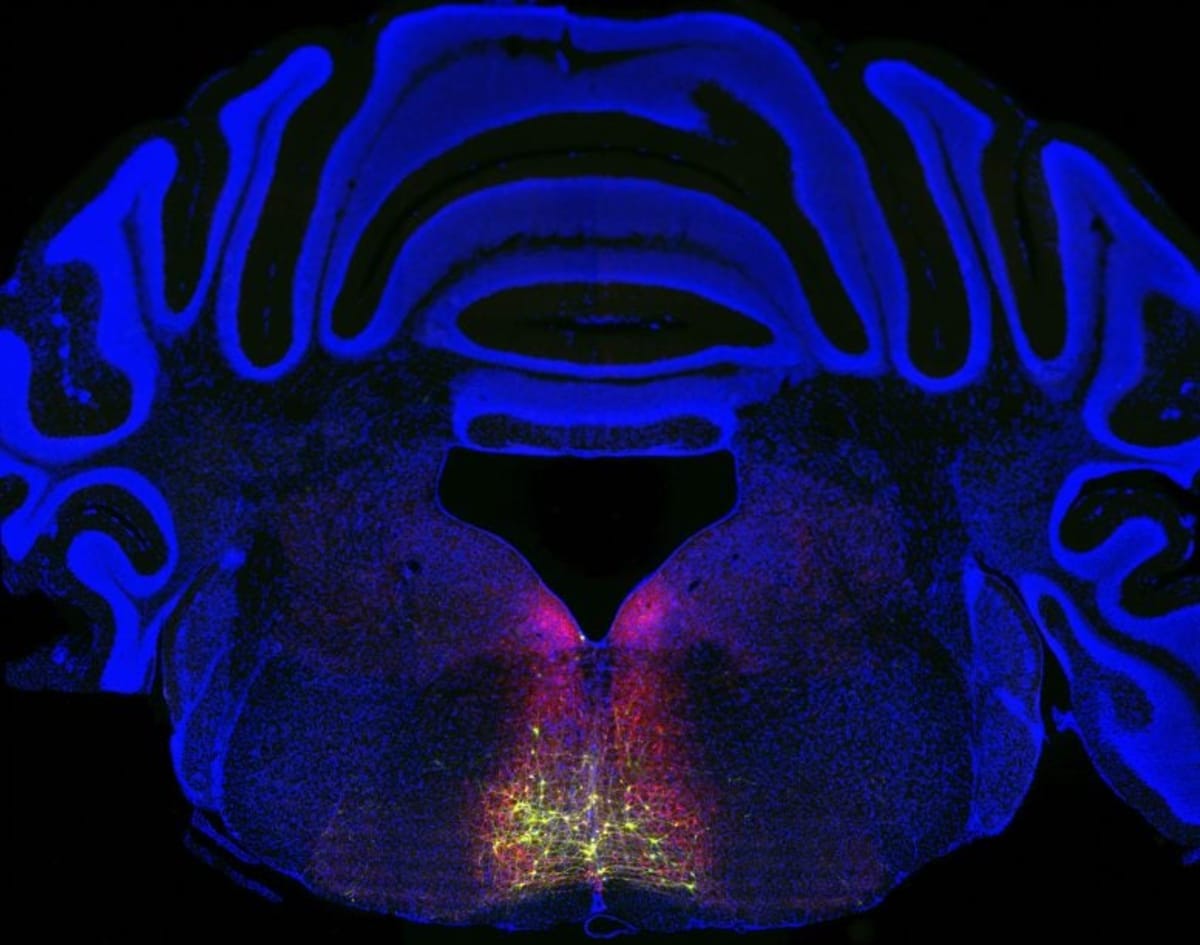
The research started with neurons in a brain region called the rostral ventromedial medulla. Using fluorescent markers, scientists traced a loop that starts in the spinal cord, passes through the thalamus and cortex, then circles back to the spinal cord. This circuit only activates after injury or inflammation, never during normal pain experiences.
When researchers chemically switched off this pathway in mice showing chronic pain symptoms, the animals stopped overreacting to gentle touch. Their hypersensitivity vanished, but they could still sense harmful stimuli normally. The opposite happened when scientists activated the circuit in healthy mice. Just turning on these neurons created lasting pain sensitivity that persisted for weeks.

The findings explain why chronic pain feels so different from a warning signal. In chronic conditions, the brain misinterprets ordinary sensations like light touch as painful threats. This sensitization often leads to mental health struggles and increased risk of opioid dependence, making safer treatments desperately needed.
The Bright Side
This research doesn't just identify a problem. It hands scientists a specific target for new medications that could block chronic pain signals without touching the protective pain system. Chen's team is now hunting for the molecular switches that activate this circuit, work that could lead to precise drugs within years, not decades.
The researchers are also analyzing genetic data from people with chronic pain to confirm the same mechanism exists in humans. Early signs suggest it does, which means treatments developed from this discovery could translate directly to patient care.
The breakthrough emerged partly from the NeuroChoice Initiative, a project studying addiction biology and the risks of prescription opioids. By offering a path to pain relief that preserves normal pain function, this circuit could help millions find comfort without the dangers that have fueled the opioid crisis.
One mystery remains. Why would evolution create a circuit dedicated to amplifying pain? Chen suspects it might help the brain detect internal damage, since brain tissue itself lacks pain sensors. For now, that question waits for future research. But for people counting years in pain instead of days, this discovery already changes everything.
More Images
Based on reporting by Google News - Scientists Discover
This story was written by BrightWire based on verified news reports.
Spread the positivity!
Share this good news with someone who needs it


