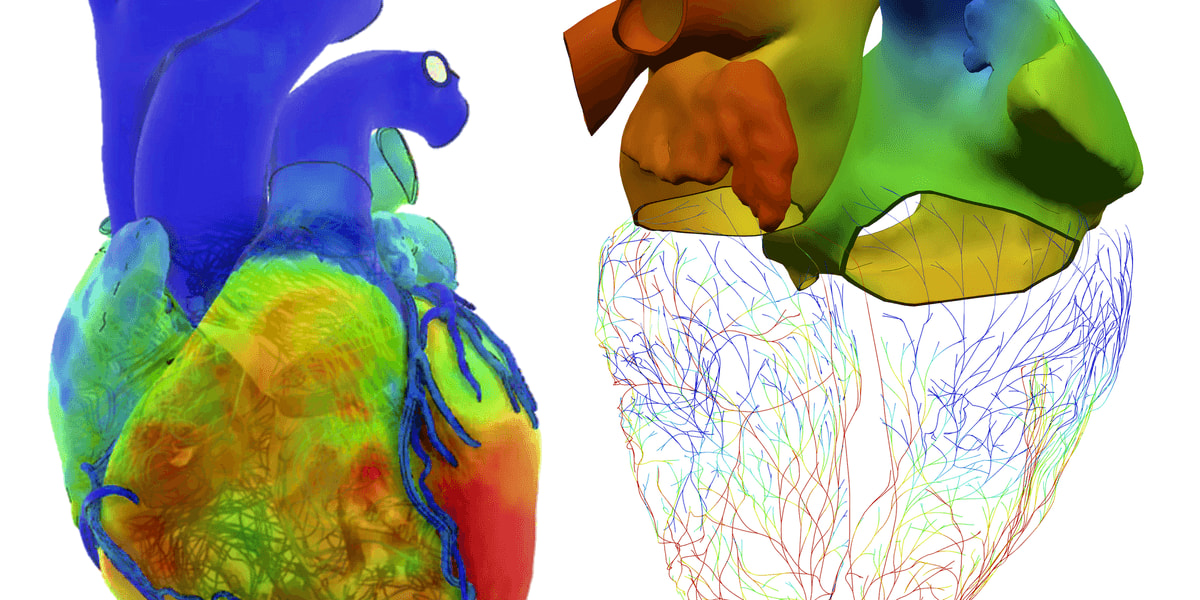
Virtual Heart Models Save Lives at Boston Children's Hospital
A surgeon rehearsed complex heart surgery dozens of times on a digital twin before operating on a real child. Since 2019, nearly 2,000 procedures have been guided by this groundbreaking technology.
A cardiac surgeon walked into Boston Children's Hospital in May 2019 already knowing exactly how to rebuild a young patient's heart. He had practiced the intricate procedure dozens of times on a perfect digital replica of the child's unique anatomy.
The surgical team had spent weeks building a fully functioning virtual twin of the child's heart from MRI and CT scans. This wasn't just a 3D picture but a living digital model that mimicked real blood flow, pressure, and muscle movement.
The patient faced a rare heart defect with holes between chambers that strained the lungs. No textbook could guide the doctors through this specific case. But the virtual twin let them test different surgical strategies in advance, predicting exactly how each cut and stitch would affect this particular heart.
The surgery succeeded completely. The child's heart now works properly, rerouting blood flow just as the digital model predicted.

This technology comes from the Living Heart Project, launched in 2014 by engineer Steve Levine. His own daughter Jesse has a rare congenital heart condition, and watching her face diagnostic uncertainty sparked a powerful question: Why can't we simulate the human body the way we simulate cars and planes?
Levine had spent his career helping engineers build digital models of complex machines. He realized the same physics that predicts how a vehicle performs could predict how a heart behaves. Yet most medical decisions still rely on static images and best guesses rather than dynamic simulations.
The approach has transformed care at Boston Children's Hospital. Since that first patient in 2019, virtual twins have guided nearly 2,000 procedures. Surgeons now walk into operating rooms with detailed rehearsals complete, knowing which approach will work best for each unique patient.
The Ripple Effect: The Living Heart Project now includes over 150 member organizations across 28 countries. Multidisciplinary teams regularly use virtual twins not just for hearts but for other vital organs too. Patients who once faced uncertain outcomes now benefit from surgeons who can practice on their exact anatomy before making the first incision.
The technology bridges a gap that has existed for generations. Early physicians understood the body through physics, seeing the heart as a pump and the lungs as bellows. As medicine evolved, biology and chemistry took center stage while physics fell away. But for patients with structural heart problems, outcomes depend on mechanics, not medications.
Virtual twins are bringing physics back to medicine, one life-saving rehearsal at a time.
More Images
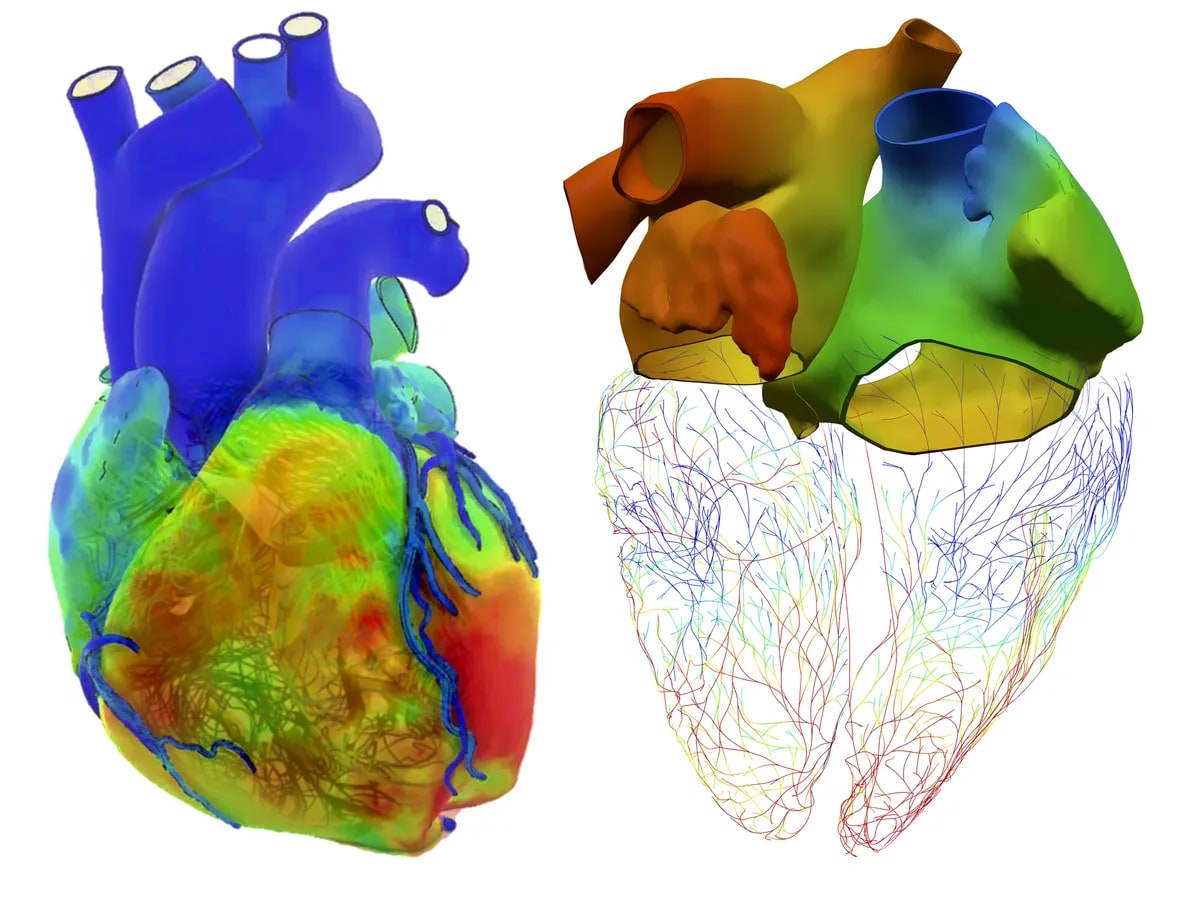
Based on reporting by IEEE Spectrum
This story was written by BrightWire based on verified news reports.
Spread the positivity!
Share this good news with someone who needs it


